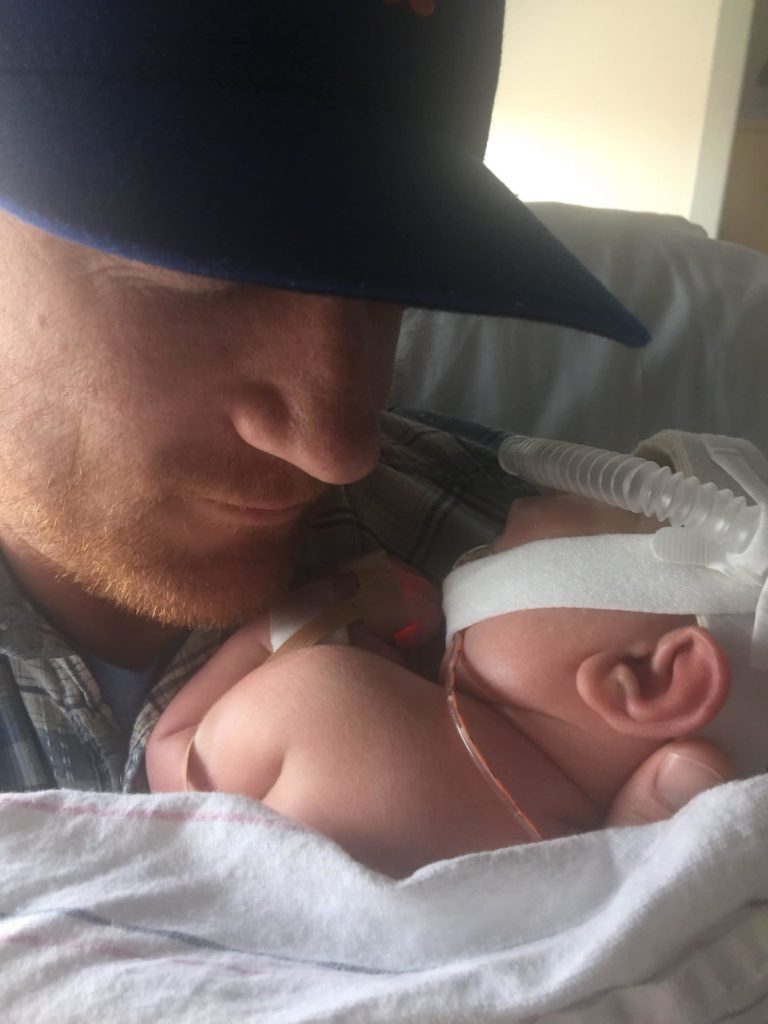
It was the second week in the NICU when we started to realize that we weren’t the typical family. Our first child, Grey, had suffered a severe brain injury at birth (known as hypoxic ischemic encephalopathy), and he was still fighting for his life. He hadn’t yet woken up or opened his eyes, he still was on breathing support, and he had a chest tube. We were getting visits from cardiology, neurology, and respiratory techs. We were awaiting the results of his MRI, which could tell us how severely his brain was damaged. Every day was a whirlwind of heartbreak and hope, and my wife and I were numb from the raw emotion and forced acceptance.
We shared a corner of the NICU with a young mother and her preemie, and she approached us one day for the first time. “He’s a big boy! When can you take him home?” The nurses and therapists had already commented on how big our son was, even though his weight was in the mid-percentiles and totally typical for a full-term baby. It was her question about taking him home, though, that gave us pause.
“We don’t know, yet,” we answered—and we really didn’t. We had been so overwhelmed with worry about our son’s critical condition that we hadn’t let ourselves even consider when he might be able to come home. We weren’t even sure that he would come home with us. After that moment, we started to notice that pretty much all of the other families were either parents of a preemie, or only in the NICU for a few days. No one wants to have their baby taken to the NICU, and the fear of being there is something that all parents who have can relate to. For us, though, this was the beginning of a long-term, life-altering diagnosis.
We got to know the routine of the place. We knew exactly how to scrub up to the elbows, and would admonish our friends and family who visited and didn’t know to turn off the faucet using a paper towel. We learned that nothing touches the floor, and that phones and handbags don’t go in the his crib. We knew where the good coffee was, where the 4oz. cups of apple juice were, and which security guards would always ask us for a visitor’s pass, even if they’d already seen it five times that day.
We met amazing doctors, nurses, and therapists. There was Karen, the nurse manager, who made us hold Grey on his fifth day of life even though we thought we might break him or rip out one of the many wires or tubes that were keeping him alive. There was Liz, the attending doctor who told us that one of us would have to quit our jobs to be able to properly care for him, but also gave us hope that Grey would always respond to our love and care. There was Michele, the nurse who made us change his diapers and give him sponge baths at a time when we were feeling like helpless spectators instead of parents. There was Sarita, the physical therapist who showed us how to stretch Grey and give him a massage. There was Lori, the respiratory tech who patiently showed us how to suction Grey through his nostrils, and took care of him overnight while we weren’t there.
Grey slowly got more stable, and after a month, we were moved to a rehab hospital next door. He is two and a half now, and still severely affected by his injury. He still receives care at the hospital where he lived for his first month, and the smell of the soap in the restrooms still brings me back. During that month, I cried more than I ever have. I loved my wife and my family more than I ever have. We had our hearts ripped out and found a way to stitch them back together because our baby boy needed us. For better or worse, it was the most memorable time of my life. Were we the typical NICU family? No, but it wasn’t just what Grey was facing that made us feel different. It was how these amazing professionals saw a family in distress and rose to the occasion to give us their compassion, love, and care.
Nick Burton serves as VP of outreach for Hope For HIE, a parent-based, non-profit resource for families whose children have been diagnosed with hypoxic ischemic encephalopathy. Hope for HIE is deeply committed to providing comprehensive, personalized support, and represents a variety of outcomes – from unaffected through loss.